The operation that is commonly called "full knee replacement," or "total knee arthroplasty," consists of resurfacing of the knee joint. It is not a replacement of the entire knee structure.
In other words, "knee replacement" is surgery in which a layer is removed from all three knee bones using battery-powered saws, chisels, hammers, etc., followed by covering of the surfaces with artificial material (metal and plastic).
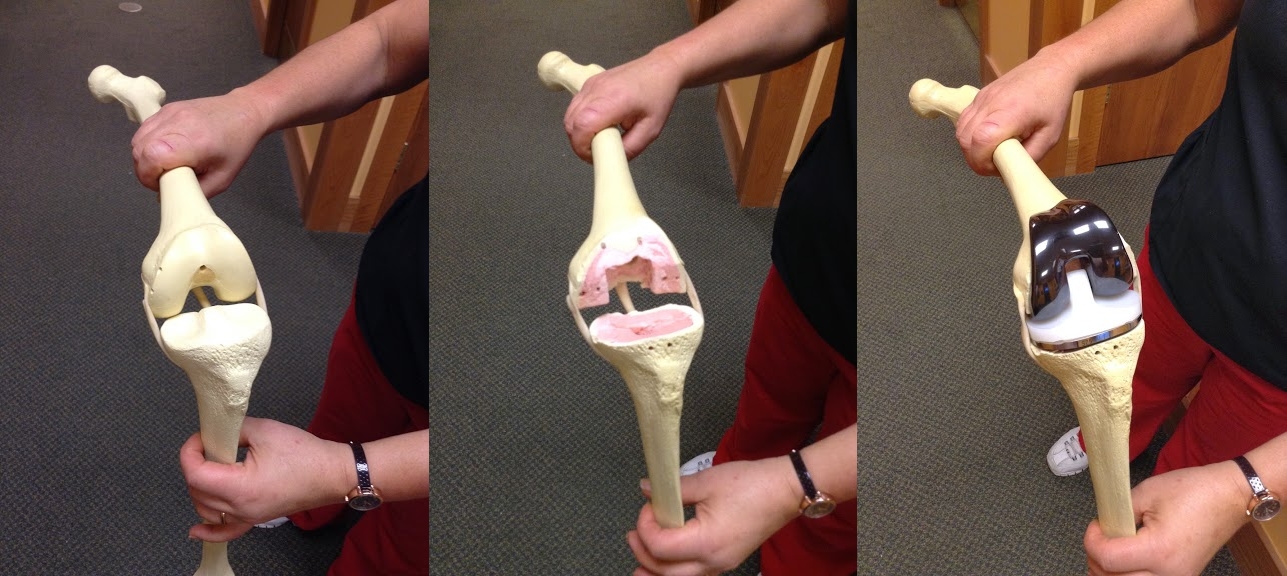
The bone model below demonstrates a left knee replacement; the kneecap is not shown. To the left is the uncut femur and tibia. In the middle, the bone surfaces have been removed. To the right, the bone ends are covered with the artificial prosthesis.

The knee joint
Three bones meet at the knee joint.
- The femur starts above at the hip and ends as the upper bone at the knee.
- The tibia starts at the knee, and ends at the ankle.
- The patella, the kneecap, is part of the quadriceps muscle; it serves to transmits the quadriceps muscle forces to the tibia, so that one may be able to straighten the knee, climb stairs, stand from squatting, etc.
Is there more than one kind of knee replacement?
Yes. Below a few variations on the theme.
- UKA, unicompartment knee arthroplasty, or partial knee replacement is appropriate for some patients with limited disease. UKA has higher odds of needing an early redo surgery, but when UKA works, the knee feels more normal than with a complete replacement.
- TKA, total knee arthroplasty; this is what is usually meant by "knee replacement". In the US, typically the operation involves resurfacing of the patella, but in Europe the patella is usually left alone.
- PS, posterior substituting. This refers to a kind of TKA. This is a design philosophy for knee replacement prostheses that does away with the need to have a functional PCL (posterior cruciate ligament).
- CR, cruciate retaining. This is the other kind of knee replacement technique. Its success depends on having a strong, functional PCL.
- Cemented vs uncemented knee replacement: most surgeons use PMMA to fix the artificial parts to the bone. Cement allows for immediate weight bearing.
- The terms computerized, navigated, MRI aided, prenavigated, PSI, Makoplasty, etc., refer to certain newer tools and methods that the surgeon may use to help measure and make the bone cuts. The fundamental nature of the operation does not change.
- Last but not least: there are many manufacturers of knee replacement prostheses. The "big 3" of the knee prostheses are Zimmer, DePuy, and Stryker. Each of these manufacturers offers more than one different model. The situation is similar to the car market, where there is an abundance of choices, each with its own advantages and drawbacks.
What is the best method for replacing a knee?
There are thousands of scholarly papers on the topic, which often contradict each other, or are just somebody's opinion or bias (as opposed to accepted truth). Nobody can say for sure. The joint arthroplasty registries from the socialized medical systems of Europe provide some of the best data to help one decide what is good and what is not so good.
For simple uncomplicated knee replacement cases, I routinely use:
- Standard medial para-patellar arthrotomy.
- Zimmer Nexgen CR prostheses.
- Intramedullary rod alignment for the femur, extramedullary for the tibia. Low threshold for intramedullary rod for the tibia as well.
- I use cement, loaded with antibiotic, every time.
- Meticulous wound closure.
Typical course after a knee replacement operation
- I perform this operation with spinal anesthesia.
- Patients usually spend 1-2 nights in hospital.
- Immediate weight bearing.
- Physical therapy in hospital: full extension, at least 90 degrees of flexion, walking with walker starting immediately.
- Physical therapy after discharge must continue without interruption.
- Follow up at
- 2 weeks after surgery for staple removal
- 6 weeks after surgery
- 3 months, 6 months, and 12 months after surgery
- Expect to discontinue walker at 3 weeks.
- Most patients are able to walk comfortably by 6 weeks.
- The knee can be warm and can look swollen for 1 year after surgery.
- The best predictor of post-operative flexion is preoperative flexion. Multiple statistical studies have shown this, and it is not realistic to expect to bend the knee fully after surgery, if you could only bend the knee 45 degrees before surgery.
- The ability to kneel down is affected by total knee replacement. This is a limitation of current technology.
- I routinely advise antibiotics, typically amoxicillin 2 g, before dental and other invasive procedures, for life.
Risks of knee replacement
Knee replacement is a routine operation, but it is a violent operation during which motorized power tools and heavy hammers are used. It is not risk free and complications can occur.
Here is a list:
- Death. A heart attack can be brought on by anxiety before or after, by blood loss, by pain, by a blood clot.
- Infection. On average, in the US there is 1 infection for every 100 of these operations. Infection after TKA is a most serious complication. It is often necessary to remove the knee replacement, try to cure the infection, and then reinsert a prosthesis at a later date. Infection, in the best case scenario, makes for a very bad 6 months or so. Even when the infection is finally cured, the outcome expected is less than it would have been without an infection. Unfortunately, there is no sure way to prevent an infection.
- Amputation, limb loss. It happens very rarely in the US, the culprit is usually infection.
- DVT and PE. 1-2 % of patients suffer from this complication.
- Loosening and wear of the prosthesis.
- In 100% of the cases, there is some numbness from the incision and sacrificing of the infra patellar branch of the saphenous nerve.
- On rare occasions there may be temporary numbness and ankle paralysis from stretching of the peroneal nerve. Foot paralysis after TKA is very much possible and has been described in literature.
- Across the US, statistics show that approximately 15% of patients who receive knee replacements are not entirely happy with them for one reason or another.
How long does a knee replacement last?
10 and 15 year survival rates are approximately 95% and 90% respectively. This means that out of 100 implanted prostheses, 15 years later 10 of those prostheses have failed for various reasons, including infection, mechanical wear, loosening, fracture, etc.
What happens when a prosthesis fails?
Depends on the reason of failure. Most times it is possible to do revision surgery and reinsert a new part, or a whole new prosthesis.
How is knee arthritis diagnosed?
Knee arthritis is diagnosed by xray.
The following picture shows xrays of patients with different grades of arthritic disease. Grade 1, the mildest, has "doubtful" findings on xray. At the other end of the spectrum grade 4 has "bone-on-bone" disease, deformity, large osteophytes, and so on.
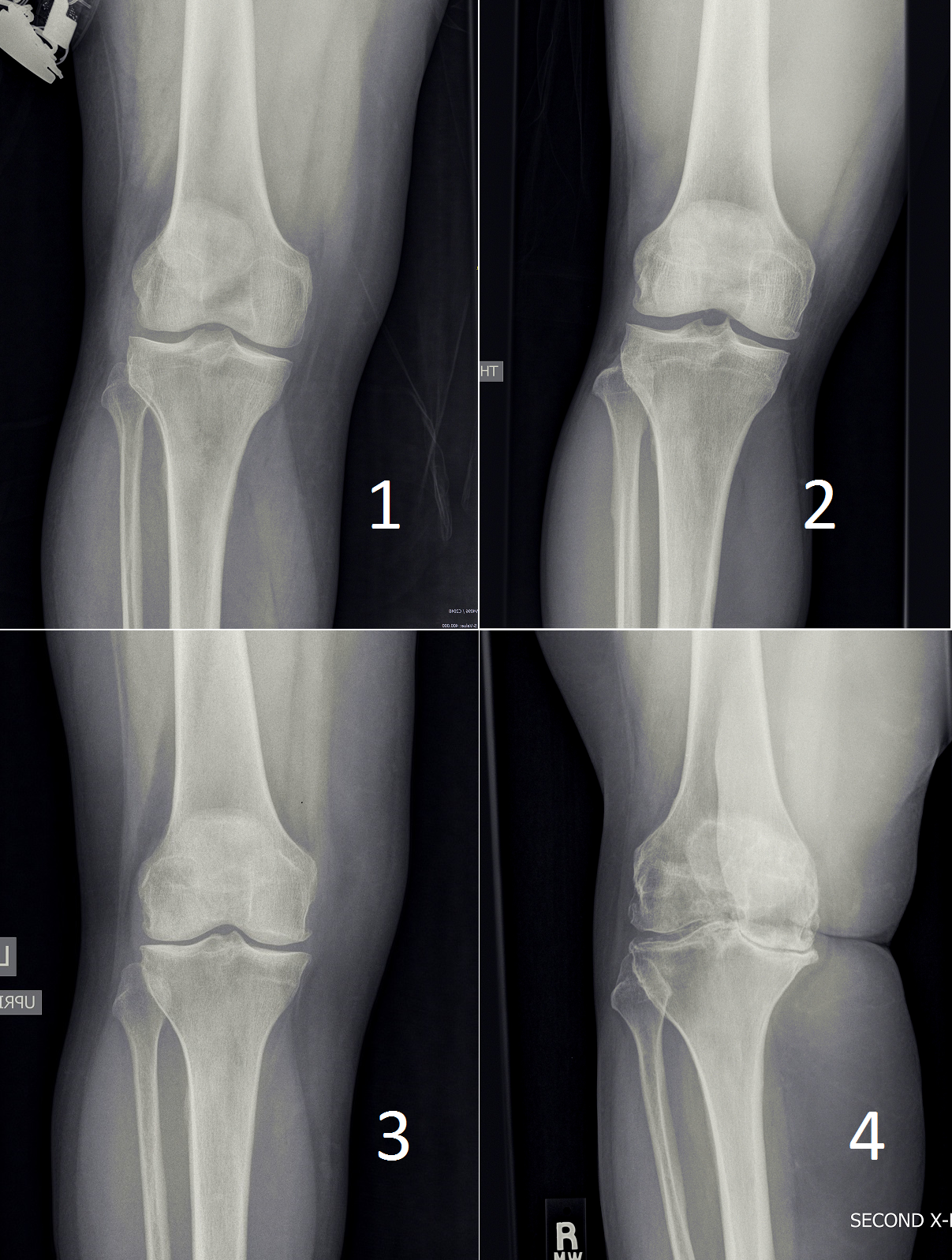
An MRI does not help in the typical arthritis patient. It is an unnecessary expense of time and treasure, and should be avoided. (There are, of course, individual circumstances and exceptions.)
Are there alternatives to knee replacement?
At this particular moment in time, in the year 2013AD, if a knee joint has become arthritic, there is no way to stop or reverse the process. Arthritis is progressive, and tends to get worse with time. This sounds hopeless, but in reality it is no worse than many other human ailments. On the positive side, treatment and pain relief is possible.
These are the options:
- If pain is tolerable, no specific knee intervention is needed.
- "Activity modification": this implies doing less of whatever it is that makes the knee hurt.
- NSAID medications: if Tylenol does not help, it is worth trying naproxen, or ibuprofen, or mobic.
- Needle aspiration of knee effusions and judicious use injections oftentimes help tremendously, but of course, they do not stop the disease.
- Surgery: arthroscopy or knee replacement.
- Unfortunately, arthroscopy is not very effective for arthritis. Unless there is a specific treatable issue such as a loose body, or a large meniscal tear that acts as a loose body, or some other such problem, you can expect arthroscopy to not help a lot with the arthritic pain. Understanding that it probably won't solve the problem, one may still wish to try arthroscopic surgery because it is a much smaller operation.
- Knee replacement, more properly called "arthroplasty" is the definitive treatment available today for severe painful knee arthritis.
Case study
Before and after pictures of a knee replacement of a very arthritic knee that I treated with knee replacement.
